Risk perception
Expert perception

Health experts do not view the risks associated with a medical procedure (such as vaccination) in the same way as members of the public (parents, patients and vaccinees).
Experts understand risks in terms of numerical values and rates: for example, this table compares the risks of death due to three vaccine-preventable diseases and the risks of adverse events following immunization with the approved vaccines.
Risks of illnesses and risks associated to the corresponding vaccines
| Measles | Death:
|
|---|---|
| Diphtheria | Death: 1 in 20 cases. |
| Tetanus | Death: 25 – 70 in 100 cases overall. (10 – 20 in 100 cases with good intensive care management.) |
| Measles vaccine | Encephalitis or severe allergic reaction: 1 in 1,000,000 cases. |
| DTP vaccine | Continuous crying, then full recovery: 1 in 100 cases. |
| Tetanus toxoid vaccine |
|
Public perception
In contrast to the perception of experts, parents, guardians and vaccinees rather want to know whether they or their child could be the "one in a million" who develops encephalitis following immunization with measles vaccine.
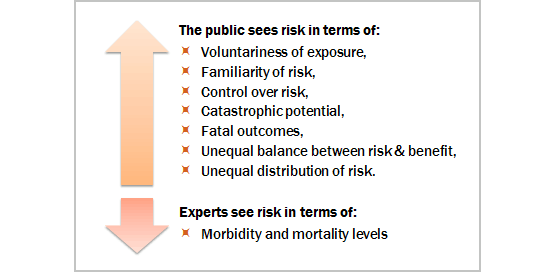
Other factors that may influence the way public tends to see risk, include:
Negligence of the danger of the disease
Most adults in high-income countries with high vaccination coverage have never seen a case of measles or any of the other vaccine-preventable childhood diseases. As a consequence, they may underestimate the probability of harm if the disease does develop.
Influence by individual context
The public is likely to perceive risk in broad religious, social or personal contexts. For example, some will distrust the medical system due to a personal prejudice against "experts" and a desire not to be influenced by them; others will uncritically accept all instructions from health workers because they feel intimidated or inferior.
Aversion to medicine
Adverse personal experiences from the past (e.g. the memory of a painful injection or a sore/swollen arm) may also negatively influence attitudes to vaccine-associated risk. The thought of being injected with a foreign substance derived from disease-causing organisms can induce fear and dread. Clients may feel reluctant to come to a clinic or other health facility, or to bring their children if the environment feels intimidating and the health workers are not reassuring or welcoming.
For all these reasons, it is important to understand the concerns of your target audience and the different approaches required to communicate effectively with persons planning to receive a vaccine, the public and your expert colleagues.
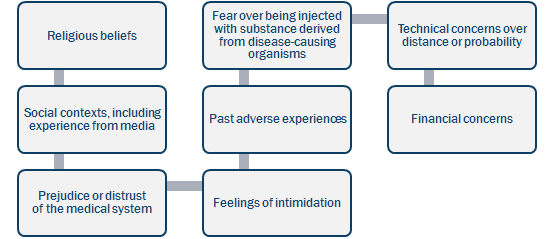
Concerns of the target audience
There are some common misconceptions about vaccination that are often cited by concerned parents as reasons not to get their children vaccinated. If staff can respond to these with accurate rebuttals perhaps they may not only ease parents' minds but discourage them from taking other anti-vaccine "facts" at face value.
These are six of the most common misconceptions that may occur among persons that receive a vaccine. Information to counteract these beliefs in your communications can be boud at: who.int/immunization_safety/aefi/immunization_misconceptions.

